Cord Blood Donation and Storage
A child’s birth is a gift of joy to a family and could offer the gift of life to others. Umbilical cord blood is a rich source of blood stem cells that are crucial in life-saving transplants, instrumental in groundbreaking medical research, and present a new pathway for treating diseases now considered untreatable. Cord blood donation allows stem cells to be easily collected to treat more than 70 diseases, including blood cancers and sickle cell disease, in 35,000 patients worldwide.
If you are considering to umbilical cord blood banking for public use, you should be aware that your blood will be tested for both genetic abnormalities and infectious diseases. Since most banks require mothers to sign up for donation between the 28th and 34th week of pregnancy, families must decide to donate ahead of time.
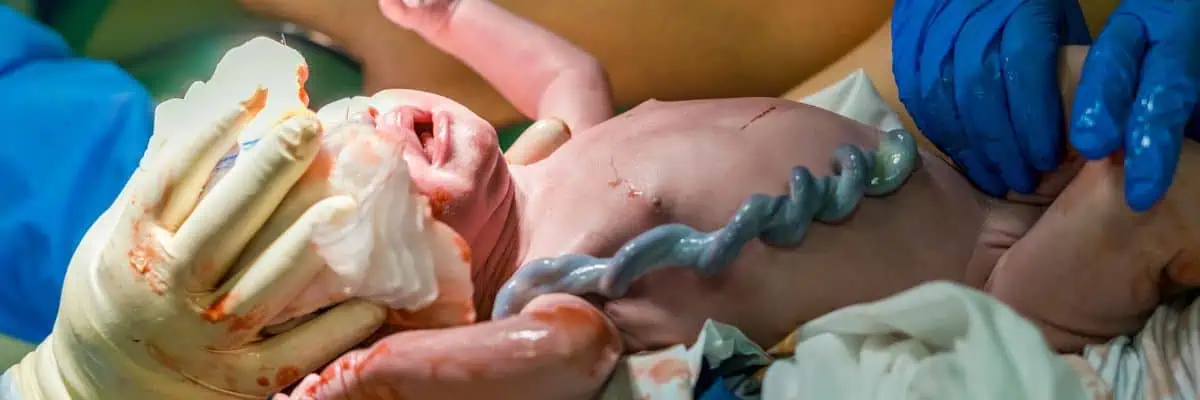
Cedars-Sinai Offers for Options to Families Wanting to Donate or Store Cord Blood
Cedars-Sinai offers the most comprehensive options for banking and storing cord blood — the few ounces of blood left in the umbilical cord and placenta after delivery — through an exclusive agreement with CORD:USE, a leading cord blood bank.
- Public Bank: Free anonymous donation to CORD:USE’s public cord blood bank: if your donated cord blood meets the criteria, it will be made available to patients who need a transplant.
- Private Bank: Private cord blood bank for family use through CORD:USE. The cord blood will be collected and stored for a fee to be reserved for a family’s exclusive use. This option is fee-based.
- Private bank + storage for possible generation of induced pluripotent stem cells (iPSCs) in the future: A portion of your child’s stored cord blood is isolated for the possible later generation of iPSCs. The iPSCs are not generated unless requested or needed. The isolated portion can be converted to iPSCs at Cedars Sinai at any time for possible future therapies. The fee for this option is the same as the cost for private banking + an additional $65.
- Private bank + generation of stem cells for future disease therapies: After the cord blood is collected and tested, a portion is converted to iPSCs at Cedar-Sinai and is stored in the medical center. The iPSCs at Cedar-Sinai may offer families timely access to important future disease therapies if needed. The fee for this option is the same as the cost for private banking + an additional $5,650.
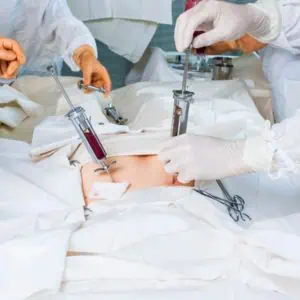
How is Cord Blood Collected?
Cord blood collection takes place after a baby is born, and the umbilical cord has been cut. It is then collected by a health care provider. The collected cord blood is packaged and shipped to CORD:USE and is processed by the laboratory within 48 hours of collection. There are no health risks to the baby or mother from cord blood collection.
Why is Cedars-Sinai Exclusively Partnering with CORD:USE?
Families face hundreds of decisions when they learn they will have a baby. Several companies offer cord blood banking services, but not all of them use the same methods and practices to store the cord blood. Experts from our Department of Obstetrics and Gynecology and from the Cedars-Sinai Regenerative Medicine Institute vetted a number of companies and found that CORD:USE exceeded their expectations in the quality of their service and best practices for storing cord blood. CORD:USE is one of the few companies offering both an accredited public cord blood bank and private cord blood banking services. It uses the highest quality processes and advanced technologies to increase the likelihood that the stored blood will have the maximum number of viable cells when it is needed for medical use. In addition, CORD:USE and experts at the Cedars-Sinai Regenerative Medicine Institute have developed a protocol that will allow a portion of the cord blood to be isolated for future stem cell generation.
Can I do Both Delayed Cord Clamping and Cord Blood Banking?
Yes. If needed, obstetricians may wait 30 seconds to a minute or more before clamping or cutting the umbilical cord, which is known as delayed cord clamping. Obstetricians and families do not need to alter their care plan for the mother or baby to accommodate cord blood collection.
When is Cord Blood Used for Transplantation?
Cord blood is one of three sources of stem cells used in transplants to treat patients with blood cancers and other hematologic malignancies. The other sources are bone marrow and peripheral blood stem cells. One of cord blood’s many advantages is that it does not cause as severe or as frequent rejection disease as seen with bone marrow.
- Cord blood is an especially important resource for those patients who do not have an immediate family member who is a match to donate bone marrow or stem cells for transplant. Published studies have found that cord blood units do not need to match a patient as closely as donations from bone marrow or peripheral blood to be transplanted successfully.
- Cord blood is also helpful when a patient needs a transplant quickly. Because the units are stored and readily available, they may be a better option for a patient who cannot wait weeks or months to find a suitable bone marrow donor.
- Lastly, these units are especially important for those from diverse racial and ethnic backgrounds who have difficulty finding a suitable match through the National Marrow Donor Program Bone Marrow Registry and other bone marrow donor registries.
More than 25,000 patients around the world have received cord blood transplants because parents chose to donate their baby’s cord blood to public cord blood banks
What is the Benefit of Donating to a Public Bank?
Any patient in need of a blood stem cell transplant to treat a blood cancer or hematologic malignancy has access to cord blood units made available by the public bank through the national cord blood registry. There is no cost to families because the public cord banks pay for the processing, testing, and storage of donated cord blood. Once the unit is listed in the National Cord Blood Inventory, there is no guarantee that it will be available specifically to your family, as it may have already been used in a transplant. Blood for public cord blood banks is collected under stringent quality standards to ensure the blood unit is used for transplant. Those units that do not meet these standards may be used for research or be discarded.
Should Our Family Consider Storing Cord Blood for Private Use?
While cord blood has been a successful treatment for a number of diseases and immune disorders, there are no accurate statistics on the likelihood of children someday needing their own stored cells. It is not known for exactly how many years the blood may be stored and remain viable. Thus far, we do know that Hal Broxmeyer, Ph.D., credited with being a founder of the field of cord blood and who is the founder of CORD:USE’s family cord blood bank, tested units that were cryogenically frozen for 23 ½ years and all samples were viable.
Donation to Public Banks or Private Banking
Historically, the chance of using one’s cord blood has been low. The American Academy of Pediatrics and American College of Obstetricians and Gynecologists recommend families donate cord blood for use in public banks in most cases. Private banking should be considered for family use when there is a full sibling in the family with a condition that could benefit from cord blood transplantation — as siblings have a 25 percent chance of being a match. The academy discourages private storage of cord blood as “biological insurance.” Families should discuss the cord blood donation with their doctor well before the delivery of the newborn.
Some Patients Cannot Use Their Own Stored Blood
Families should also be aware that for some blood cancers and malignancies, such as leukemia, a patient’s own stored blood most likely could not be used for treatment as those blood stem cells would have the same mutation that caused the disease. However, there are currently clinical trials being performed to treat conditions and diseases such as diabetes, other autoimmune diseases, autism, cerebral palsy, stroke, and spinal cord injury could significantly increase the likelihood of using one’s cord blood.

















