What is a Cesarean section?
A Cesarean section, or C-section, is a method of delivering a baby through a surgical incision in the mother’s abdomen.
Many pregnant women prefer to give birth naturally, but your OB/GYN may recommend a C-section if certain health problems, such as high blood pressure or diabetes, make vaginal birth too risky.
Often, however, the need for a first-time C-section doesn’t become obvious until labor is underway.

When is a C-Section Necessary?
A cesarean section is performed to minimize the health risk to the mother and baby during birth. Some medical reasons increase the risk of harm during vaginal birth.
Multiple Births
Multiple births, such as twins or triplets, can be more safely delivered via Cesarean Section. If the mother is coming into pre-term labor with multiple pregnancies, or if the positioning of the fetuses is not ideal, the doctor may recommend a C-section. The greater the number of fetuses, the greater the likelihood of Cesarean delivery.
Size of the baby
If delivered naturally, an especially large baby, relative to the size of the mother, could put the mother’s health at risk.
Breech presentation in the uterus
In a breech presentation, the baby is positioned to exit the cervix feet-first or buttocks-first. The vaginal birth of a breech baby may force the umbilical cord into an unnatural position, blocking the flow of oxygen to the baby during delivery.
Placenta Conditions
The placenta covering the birth canal or detaching from the uterine wall can pose a risk for hemorrhage.
Failure to dilate
If the cervix fails to dilate completely, your baby must be delivered via C-section.
Other medical conditions
A cesarean section can be used to prevent a transfer of infection from mother to baby during vaginal delivery, such as HIV or genital herpes,
It can also be used to avoid complications due to conditions that compromise the mother’s safety during vaginal delivery, such as heart disease, diabetes, pre-eclampsia, or eclampsia.
Once you have a C-section, you may be more likely in future pregnancies to have a C-section. It may be necessary to deliver your next baby via C-section unless your OB/GYN determines it is safe to continue with vaginal birth after cesarean.
What Should I Expect in a Cesarean Birth?
Cesarean section is a major surgery, and every surgical procedure carries risks. It also takes longer to recover from a C-section than from vaginal birth.
You will receive fluids and medication through an IV line during your surgery. The nurse will wash your abdomen and trim or shave your pubic hair. During abdominal surgery, it’s important to keep the bladder empty. The best way to do this is to insert a catheter – a thin tube for draining urine from the bladder – into your urethra.
Cesarean deliveries can be performed under two types of anesthesia:
General anesthesia
This is a heavy anesthetic that numbs your entire body and puts you to sleep during the operation.
Epidural block
Most cesarean deliveries today are done with regional anesthesia, such as an epidural or spinal block. This anesthetic keeps you awake while numbing you from the waist down. The medication is delivered directly through your spinal fluid through a small tube placed in your lower back.
Monitors will be placed to keep track of blood pressure, fetal heart rate, and blood oxygen levels.
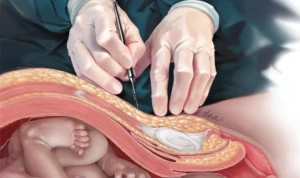
Once you are either asleep or completely numb, the surgeon will make an abdominal incision either horizontally or vertically. Your abdominal muscles may or may not need to be cut to get to the uterus.
The uterine incision is then made — The uterine wall will then be cut, usually horizontally across the lower part of the uterus (low transverse incision). Other types of uterine incisions might be used depending on the baby’s position within your uterus and whether you have complications, such as placenta previa.
The baby will be delivered through the incisions. The doctor will cut the umbilical cord and clear out the placenta, then close the incisions with biodegradable stitches.
All surgeries carry inherent risks of complications. Your surgical staff is highly trained to deal effectively with any complications in order to keep you and your baby safe. Some complications associated with C-section birth include:
- Hemorrhaging
- Blood clots, especially in the pelvis, legs, and lungs
- Infection
- Adverse reaction to a medication
- Injury to abdominal tissue, such as bladder or bowels
What to Expect After a Cesarean Section
The surgeon will clear your baby’s airways, tie the umbilical cord, and check to ensure the baby is healthy. Once you are awake and ready, you can usually hold and breastfeed your baby right away.
The nursing staff will take you to a recovery room and monitor you. As with any surgery, you may need to stay in bed and have someone help you get out of bed for the first day or two. You should expect some soreness or cramping, which can be treated with medication. A heating pad can also help with the discomfort.
You may need a hospital stay for 2-4 days following a cesarean section. Avoid putting any objects into your vagina, and refrain from sex or strenuous exercise for 4-6 weeks. During your recovery, you may experience:
- Cramping
- Vaginal discharge, bleeding or clotting for up to 6 weeks
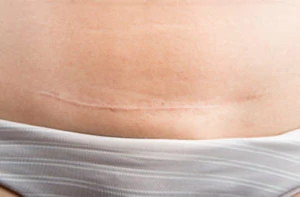
- Pain and soreness at the site of the incision
- Wound infection
These symptoms are completely normal. However, call your healthcare provider if the bleeding is heavy, your pain worsens, or you develop a fever. These may indicate a serious complication or infection.
The more C-sections you have, the higher your risk of placenta previa and a condition in which the placenta becomes abnormally attached to the wall of the uterus (placenta accreta). You’re attempting vaginal birth after cesarean (VBAC),and there’s concern about a uterine rupture at the site of your previous c-section incision.
Why Choose Dr. Aliabadi
As one of the nation’s leading OB/GYNs, Dr. Thaïs Aliabadi offers the very best in women’s health and well-being. With her warm, professional team, Dr. Aliabadi supports women from puberty to pregnancy, childbirth, menopause, and beyond. She fosters a special one-on-one relationship between patient and doctor.
Highly trained and honored by the medical community, Dr. Thais Aliabadi is certified by the American Board of Obstetrics and Gynecology and a Diplomat of the American College of Obstetrics and Gynecology. She implements the most advanced, state-of-the-art technology and treatment options.
Dr. Aliabadi specializes in up-to-date, minimally invasive surgical techniques for fibroids, polyps, and endometriosis, promising her patients shorter recovery times, reduced pain, and the least interruption to their daily lives.
We also invite you to establish care with Dr. Aliabadi. Please make an appointment online or call us at (844) 863-6700.
















